All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit Know ALL.
The ALL Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the ALL Hub cannot guarantee the accuracy of translated content. The ALL Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The ALL Hub is an independent medical education platform, sponsored by Amgen and Autolus. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View ALL content recommended for you
Antibiotic treatment is associated with decreased response to CAR T-cell therapy
The health and diversity of the gut microbiome has been recognized to play a role in numerous health conditions. In particular, a link has been noted between the diversity of the microbiome and successful treatment with immunotherapies. One previous study noted a decrease in the alpha diversity, a measure of the richness of microbial species, within stool samples after allogeneic stem cell transplant (allo-SCT).1 In addition, an increase in the proportion of Enterococcus faecium in the stools of patients undergoing allo-SCT has been associated with an increase in graft-versus-host disease-related mortality and reduced overall survival (OS).2
During the 3rd European CAR T-cell Meeting, Viktoria Blumenberg presented a talk on the association between diversity of the gut microbiome and response to CAR T-cell therapy.3 Her group hypothesized that treatment with antibiotics prior to CAR T-cell therapy injures the gut microbiome, resulting in increased toxicity and a reduced response to cell infusion. This data is particularly relevant given the difficulty in distinguishing between an infection and cytokine release syndrome in these patients.
Study design3
Stool samples (n = 252) were collected from 53 patients with diffuse large B-cell lymphoma or B-cell precursor acute lymphoblastic leukemia, prior to and following infusion with anti-CD19 CAR T cells (either axi-cel, tisa-cel, or an in-house construct, HD-CAR1).
The response was assessed at 28 days after CAR T-cell treatment using 16S RNA sequencing and shotgun sequencing.
Figure 1. Study schema3
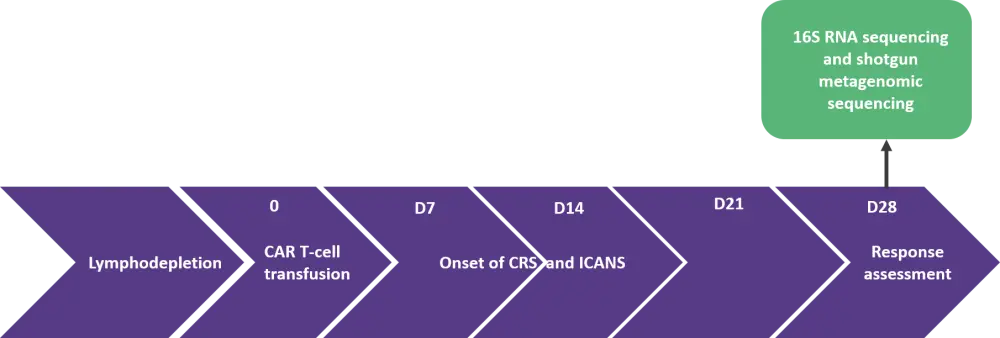
Results3
Following multivariate analysis, a significant association was found between prior antibiotic treatment and progression-free survival (PFS; HR, 21.5; 95% CI, 3.91−118.64; p < 0.001).
As antibiotic therapy affects the diversity of the microbial flora of the gut, this was investigated next. Patients undergoing CAR T-cell therapy were found to have relatively high alpha diversity prior to treatment, which decreased after CAR T-cell infusion and then subsequently reconstituted 3−4 weeks later. When considering these data in the context of antibiotic therapy, the investigators found that initiation of antibiotic treatment corresponded with the decrease in alpha diversity observed in these patients.
A positive correlation was identified between alpha diversity and treatment response; patients that responded to CAR T-cell therapy had a higher diversity at baseline, before CAR T-cell infusion, than non-responders (p = 0.016).
The team were also able to reproduce the previous findings observed in allo-SCT patients, associating lower microbiome diversity with lower OS (p = 0.004) and PFS (p = 0.01).
The number and proportion of different microbial species present was analyzed next. A high abundance of Enterococcus faecium was identified that verged on a mono-domination in some patients, confirming the results of previous studies.
Network analysis found species of bacteria that protected patients from toxicity and promoted treatment response alongside microorganisms that had a detrimental effect. The species that were negatively correlated with treatment response included Enterococcus faecium.
Conclusion
Antibiotic treatment prior to CAR T-cell infusion is associated with increased toxicity-related adverse events and inferior outcomes. Alpha diversity, which decreases after antibiotic treatment leading to an overabundance of Enterococcus faecium, is also associated with treatment response and outcome. Overall, the results of this study show that the diversity of the gut microbiome can influence toxicity of and response to CAR T-cell treatment.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

